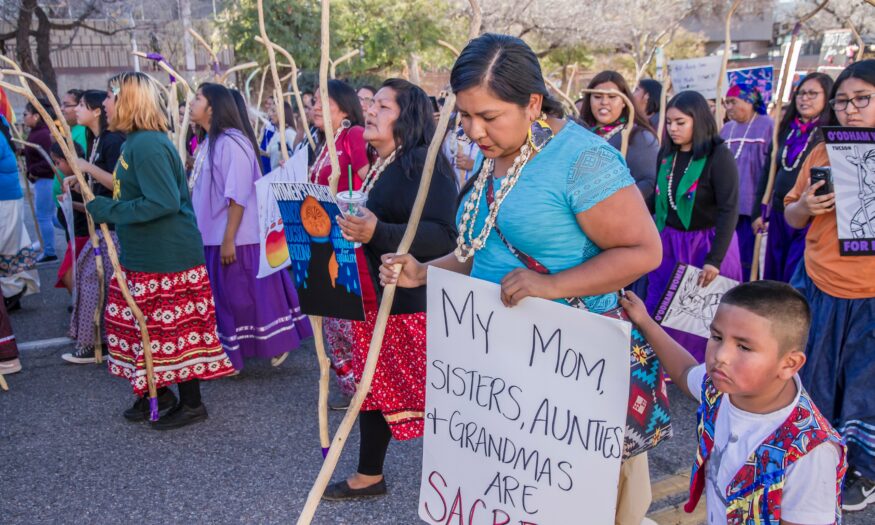PTSD in Survivors of Sexual Assault
 Illustration by Valentina Valle Rojo
Illustration by Valentina Valle Rojo
-
Topics Include:
Gender-based Violence
Intimate Partner Violence
Mental Health
The following text uses the word “pussy*” as defined by Pussypedia.
by Colleen Li
[Content Warning: sexual assault and PTSD]
What is going on?
When a bad thing happens to you, sometimes, it’s still happening even long after it’s over. Take, for example, sexual assault. Sexual assault is any sexual act where one person cannot or has not consented to sexual contact taking place. This includes, but is not limited to:1
- Attempted or completed rape (non-consensual sexual penetration)
- Unwanted or non-consensual sexual touching or contact
- Being forced to perform sexual acts, like oral sex or penetration
- Alcohol or drug-facilitated sexual assault (sexual acts done when one party was too intoxicated to give consent)
- Non-physically forced sexual assault (verbally pressured or threatened into sexual acts)
After horrible experiences like sexual assault, survivors may experience PTSD, or Post-Traumatic Stress Disorder (PTSD) which consists of intense thoughts and feelings that tend to hang around after trauma. There’s an official, clinical way of diagnosing PTSD, but really, it shows up differently in everyone. The National Institute of Mental Health has five official criterion for PTSD that must be present for at least one month:2
- At least one “re-experiencing” symptom such as flashbacks of the sexual assault, nightmares, or frightening thoughts
- At least one “avoidance symptom” such as avoiding places and things related to the sexual assault or suppressing thoughts and feelings related to the sexual assault.
- At least two “arousal and reactivity symptoms” such as: being easily startled, anxiety, feeling tense or on edge, difficulty sleeping, or angry outbursts
- At least two “cognition and mood symptoms” such as: trouble clearly remembering the sexual assault, negative thoughts about themselves and/or the world, distorted feelings like guilt or blame for the sexual assault, losing interest in previously enjoyable activities
“People might not discover their PTSD until much later on and PTSD might change over time—some months it might feel really persistent and then other months might feel totally okay. It might revisit you after years, it might come when it’s not expected, and your triggers might seem totally random.”
Triggers are specific things (could be a certain sight, a scent, being in a crowd, or a specific location) that bring back memories of the sexual assault and intense, distressing thoughts and feelings.3 Triggers are unique to the individual, and all triggers are valid. Many survivors may avoid contact with their triggers.4
How common is this?
There are statistics about rates of PTSD but they may not be accurate because many people with trauma do not self-diagnose or self-report it (just as much sexual assault goes forever unreported). The available research suggets that of the people who have experienced rape, some form of PTSD is almost a certain outcome. A 2001 study of cisgender women in the United States showed that 94% of rape victims experienced PTSD symptoms within 2 weeks of their assault. Another 47% were still experiencing symptoms within three months of their assault.5 A 2014 study of African American cisgender women in Detroit, showed that women who had experienced sexual violence were 1.6 times more likely to experience PTSD.6
People under any of these categories are at a higher risk for PTSD:7
- Have already experienced traumas
- Jobs that make potentially traumatic events more likely
- Already having mental health disorders
- Substance abuse
- Lacking support systems (like friends and family)
How can I take care of myself?
Responding to PTSD is an individual journey, and there is no “right” way to recover from trauma. Below are some potential forms of treatment and ways to cope with PTSD, but any steps taken toward recovery are valid.
“Give yourself the space to feel upset, anxious, or scared. When experiencing trauma, it’s important to have permission to feel your trauma and respond in the way that feels most authentic for you,” says Hyde.
Trauma-focused psychotherapy, talk-therapy focused on processing traumatic events, is one possible form of treatment for PTSD in general and after sexual assault. Though every experience is different, trauma-focused psychotherapy tends to last 8-16 sessions and involves visualizing, talking, or thinking about the traumatic event in order to cope with it. The most effective forms of trauma-based psychotherapy are: Prolonged Exposure (revisiting the trauma in a safe setting, allowing survivors to face their trauma and any thoughts associated with it without fear nor flashbacks);7 Cognitive Processing Therapy (analyzing the mental processes that manifested from the trauma that may be affecting daily life);7 and Eye-Movement Desensitization and Reprocessing (Prolonged Exposure along with a series of eye movements that shifts the way the trauma is processed in the brain).8
Medication is another treatment for PTSD; antidepressants can relieve symptoms of depression such as concentration and insomnia while anti-anxiety medication can treat symptoms of anxiety.7 Unfortunately, medication and psychotherapy are both expensive and not always easy to get!
Those without access can:
- Engage in physical activity and exercise.2
- Spend time with people you feel comfortable with.2
- Inform trusted people of your triggers.2
- Identify locations, people, and situations you feel comfortable in.2
- Learn more about PTSD and your symptoms. Understanding thoughts and feelings will help develop coping mechanisms.3
- Take care of yourself. Sleep, eat, and if you can, make time for self care.3
- When experiencing PTSD symptoms, do something that makes you feel more calm such as taking a walk.3
A message to survivors from the author: Sexual assault is never your fault; you don’t deserve it by any means and recovering from PTSD is fully possible. If you are in need of emergency help, please call 911.
Sources
- Basile KC, Smith SG, Breiding MJ, Black MC, Mahendra RR. “Sexual Violence: Definitions.” Centers for Disease Control and Prevention. (2018): <https://www.cdc.gov/violenceprevention/sexualviolence/definitions.html>.
- Post Traumatic Stress Disorder.” National Institute of Mental Health. (2019): <https://www.nimh.nih.gov/health/topics/post-traumatic-stress-disorder-ptsd/index.shtml>.
- “What is a Trigger?” University of Alberta Sexual Assault Center. PsychCentral. (2018): <https://psychcentral.com/lib/what-is-a-trigger/>.
- Parekh, Ranna “Predictors of PTSD Symptom Severity and Social Reactions in Sexual Assault Victims” American Psychiatric Association. (2017): <https://www.psychiatry.org/patients-families/ptsd/what-is-ptsd>.
- Ullman SE, Filipas HH. “Predictors of PTSD Symptom Severity and Social Reactions in Sexual Assault Victims” Journal of Traumatic Stress. 14(2). (2001): 369–389. <https://www.ncbi.nlm.nih.gov/pmc/articles/PMC3583013/>.
- Kate Walsh, Karestan C. Koenen, Allison E. Aiello, Monica Uddin, Sandro Galea. “Prevalence of Sexual Violence and Posttraumatic Stress Disorder in an Urban African-American Population.” Journal of Immigrant and Minority Health. 16(6). (2014): 1307–1310. <https://www.ncbi.nlm.nih.gov/pmc/articles/PMC3797217/>.
- “Post Traumatic Stress Disorder (PTSD).” Mayo Clinic Staff. Mayo Clinic. (2018): <https://www.mayoclinic.org/diseases-conditions/post-traumatic-stress-disorder/symptoms-causes/syc-20355967>.
- “PTSD Treatment Basics.” US Department of Veterans Affairs. Accessed 2019: <https://www.ptsd.va.gov/understand_tx/tx_basics.asp>.
This article was previously published in Pussypedia and is reposted with permission.
Related Stories & Conversations:
Conversations: Recommendations for Healing from Abuse
Conversations: How Past Sexual Abuse or Violence Affects Relationships